Knee Replacement Surgery
Knee replacement surgery is a very routine, well-developed procedure; each year almost a 100,000 such operations are performed in the UK.
Knee Replacement Surgery
If you’ve been suffering with severe knee osteoarthritis symptoms that aren’t responding to physiotherapy, painkillers, or other ‘conservative’ treatments, it may be necessary for you to consider surgery to replace the worn knee. This is known as a total knee replacement or a total knee ‘arthroplasty’.
Knee replacement surgery is all about improving quality of life and that means reducing pain and improving our ability to be active. It may surprise you to learn that some people can have very severe osteoarthritis in their knee, but little in the way of symptoms. Other people have moderate osteoarthritis and are really disabled by their knee pain and inability to get around.
If you’re finding that you have pain on a very regular basis that disturbs your sleep, or simply when you’re sitting in a chair, you might need to consider surgery for your knee arthritis.
Sometimes the osteoarthritis process deforms the knee into a bent shape, and many patients describe difficulty with walking, stair climbing, driving and even their ability to work. Some patients tell me that they have noticed that they’ve developed either knocked-knees or bow legs. This is a sign of significant arthritis.
Am I suitable for a total knee replacement?
When you come to clinic, I’ll be asking you lots of questions about your symptoms, the lifestyle that you lead, and what you’ve tried already to manage your knee arthritis.
I’ll then examine your knee and how you move, and we will likely carry out some imaging, such as X-rays or an MRI scan.
I’ll want to know how your knee symptoms are impacting your day-to-day life, and whether you have any past or on-going conditions. If you’re significantly overweight, or have poorly controlled diabetes, you’re not likely to cope well, or recover well from the surgery.
I may advise you that it would be necessary, and in your best interests, to reduce weight or get your diabetes under control, first.
What happens during a total knee replacement?
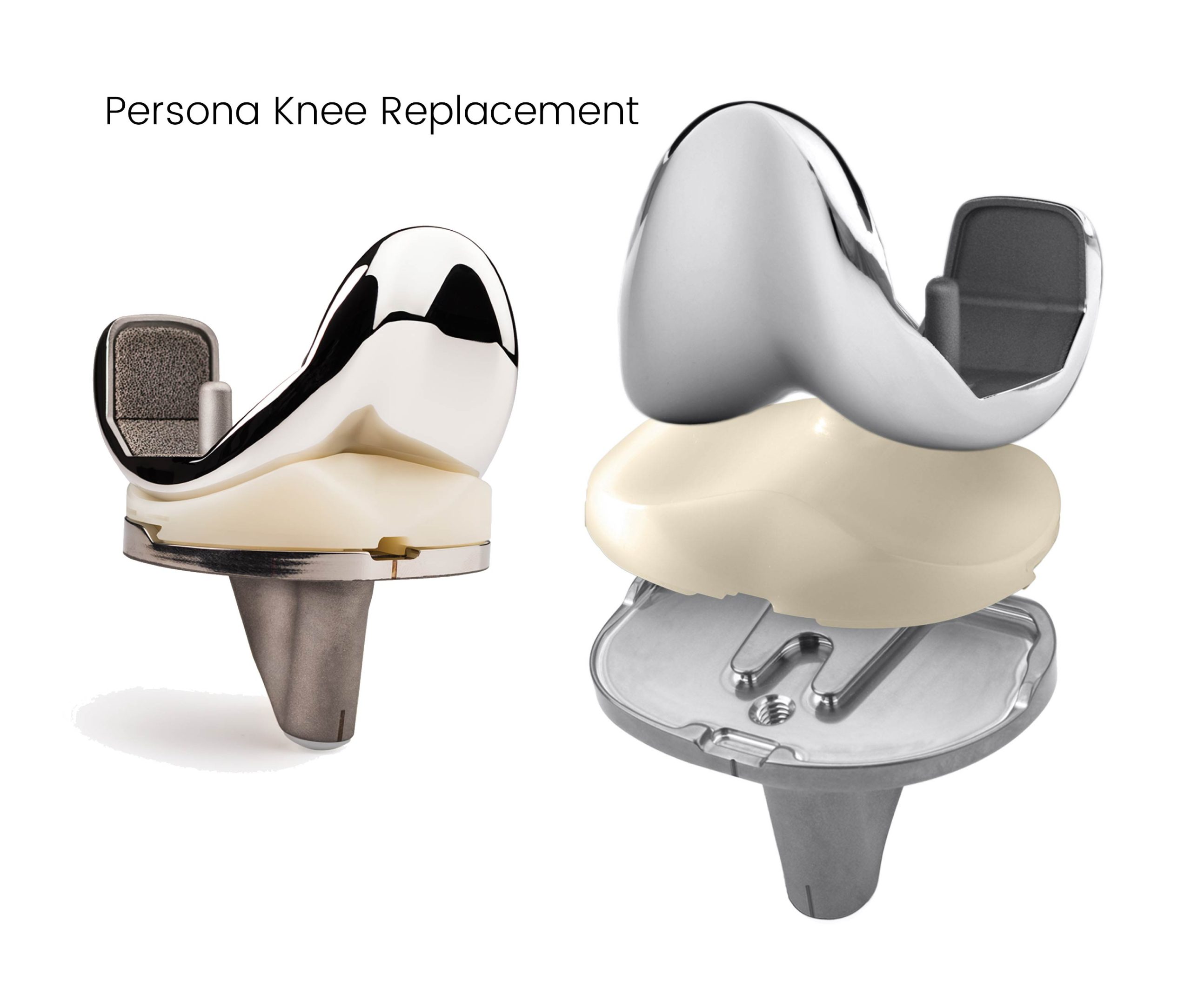
During the surgery, an incision is made down the length of the kneecap area, enabling good access into the knee. To remove the worn cartilage surfaces, cuts are made into the end of the thigh bone (femur) and shin bone (tibia); these cuts are accurately placed, using a ‘jig”. Once the worn surfaces are removed, metal implants are placed on the end of the thigh and shin bones, held in place with a special cement. A plastic polyethylene ‘insert’ separates the tibia side of the new joint from the femoral side and acts as a shock absorber and a surface upon which the new metal components can bend and swivel.
Osteoarthritis can also affect the back of the kneecap (aka patella), but studies have shown that the outcomes for patients who’ve had their kneecap ‘resurfaced’ are no different from those who don’t. In other words, I’m unlikely to recommend putting a ‘button’ on the under surface of the kneecap.
How long does it take to recover from a total knee replacement?
On the day of the surgery, you will have excellent pain control, and a physiotherapist will assist you to stand and walk on your new knee that very afternoon.
The better your muscle strength and function before surgery, the faster you will be to getting back to being fully active. Most patients will use a crutch or stick for a few weeks until they are confident enough to walk without any trace of a limp.
Whilst you can expect to have some pain after a total knee replacement, it will be different from the arthritis pain you have previously experienced. You’ll be given pain medications to effectively manage your pain in the time after the surgery.
I really encourage my patients to get moving as quickly as possible, because the people who do best are the ones who engage in the rehabilitation to get their knee moving, building their muscles, and committing to doing their physiotherapy exercises.
It’s important to understand that a new knee cannot entirely match the behaviour and movement of your own, ‘native’ knee. You’re still going to have an excellent range of movement, and the knee will operate in a very similar way to a ‘real’ knee, but there will be a few limitations.
You may find that the knee doesn’t bend quite as well. It may be a little stiff in the first few months. Most people who’ve had a total knee replacement will find it uncomfortable to kneel on the floor but adapt to this by finding other positions to get low to the ground.
What can I reasonably expect to be able to physically do after total knee replacement?
Knee replacements are artificial joints; as such they don’t wear the same way as a normal, ‘native’ joint, yet the good news is, we can expect a total knee replacement to last a ‘good’ 10-20 years.
If you choose to put a lot of impact through it, it will wear faster. Most people can return happily to cycling, golf, tennis doubles, and day-to-day activities such as walking the dog, driving, and working.
Because of the risk of loosening and mechanical wear on the new joint, I advise against running and other high impact activities.
Most people will be back to working in an office around 2 – 4 weeks after a total knee replacement, and usually back to driving around 4 – 6 weeks after total knee replacement.
If you have a heavy, manual job, you may need to be off work for longer, or undertake light duties as you are recovering.
How long will I spend in hospital?
Some patients are suitable for ‘day case’ knee replacement surgery, which means that you could expect to go home within the same 24-hour period. If that’s not suitable for you, you might expect to stay a little longer, e.g. 2-3 days.
How good are the outcomes after a total knee replacement?
There is a good deal of collective data that has been gathered, following how well patients fare after total knee replacement surgery.
In the past 30 years, satisfaction levels have stayed very constant. Around 80 to 85% of people are ‘very satisfied’ with their total knee replacement and 15 to 20% are ‘less satisfied or unhappy’ with their total knee replacement.
Interestingly, two years later, when those patients were asked how they viewed their outcome, half of them had forgotten that they weren’t happy initially.
I remind patients regularly, that it may take up to a year or more, until it feels like it’s really settled in.
If you work hard at the beginning and get the knee going and you get active, you’ll do well.
I’m occasionally asked about custom implants and ‘robotic surgery’. The implants that I use have a great track record.
Only if a person had a very great deformity within their knee would there be the need to use a custom implant.
Robotic surgery is still in its infancy; as yet, there hasn’t been any difference seen in the long-term outcome for patients who’ve had robotic surgery versus – excellently performed – tried and trusted knee replacement surgical techniques.
My goal is always to get the very best ‘kinematic alignment’ of your knee, and that means a knee that works as well as it possibly can for you.
If you’re struggling with knee arthritis and would like to have a discussion about how surgery might help you, please book an appointment.
Knee replacement complications.
A knee replacement provides excellent pain relief, improvement in function and mobility and there is a 85-90% chance of patients being very happy with their hip. It is one of the most successful operation one can have in terms of improving your quality of life. Of course, as with any operation, there are potential risks involved but fortunately, such risks are usually very small compared to the benefits of having a hip replacement.
It is important, however, that you are aware of these possible risks in order to make an informed decision about your care. It is also important to know that the recovery time following a knee replacement can take a while, as the knee after surgery can be very sore and swollen. This is quite normal and to be expected and doing your exercises to help strengthen the knee and get the knee bending and straightening after surgery is really important.
Potential risks of surgery include infection (<1%), fracture (breaking the bone), wear and loosening (the knee replacement wears out over time), damage to nerves or blood vessels, the risk of blood clots (deep vein thrombosis) in the legs or very rarely, in the lungs (pulmonary embolus), and indeed the risk of the anaesthetic.
For some patients (up to 15-20%) the knee replacement continues to be painful for some time and they are not as happy with their knee as they would like. Fortunately, with time, most patients find that their knee replacements does settle down and they become very happy with their knee. The recovery time following a knee replacement can be anything up to a year and it would be very normal after surgery for patients to have significant pain and swelling following the surgery. This will get better with time.
A great place to find out more about knee replacements can be found on the Versus Arthritis website:
https://www.versusarthritis.org/about-arthritis/treatments/surgery/knee-replacement-surgery/
The link below takes you to a great booklet all about knee replacements.
https://www.versusarthritis.org/media/23142/knee-replacement-surgery-information-booklet.pdf
Opening Hours
| Monday – Thursday | 9:00 – 17:00 |
| Friday | 9:00 – 16:00 |
At all other times, please leave a message or send an email to [email protected] and a member of the team will get back to you as the earliest opportunity.


